For Easier and More Predictable Zirconia Cementation
Premier Dental’s new self-adhesive resin cement ZR-Cem™ includes unique features to improve the definitive cementation procedure. Self-adhesive resin cements (SARC) are intended to provide the “Goldilocks” option for cementation selection, meaning they can offer the “just right” cement category for modern crown and bridge substrates. The ease of use of SARC is similar to glass ionomer-based cements but provides higher bond strengths, improved esthetics, and dual curing. Also, because SARC is resin-based it can be used for cementation of ceramic materials (eg, zirconia, lithium silicates) whereas glass ionomer-based cements are usually not recommended. Compared to adhesive resin cements SARC does not require an additional bonding step, however both require isolation for effective use.
Despite the advantages of SARC, a possible clinical challenge involves the clean-up step where all excess cement must be removed to prevent post-operative problems. Many dentists tack cure resin cements to initiate a gel phase during which the material can be easily removed with an explorer or hand instrument. However, some existing products have a very small window for tack-curing, allowing the dentist approximately 1 to 2 seconds of light curing before the material is too hard to be removed with a hand instrument. In this case the hardened material must be removed with a bur which can be very difficult and messy, especially in the posterior interproximal areas.
Fig 1. ZR-Cem™ Self-Adhesive Universal Resin Cement (Premier Dental)
Recently, Premier Dental Products Company introduced ZR-Cem™ Self-Adhesive Universal Resin Cement (Fig. 1). To help dentists prevent over curing during the critical clean-up phase, this new self-adhesive resin cement offers a tack-cure window of up to 3-seconds on both the buccal and lingual surfaces, or for dentists who do not choose to tack-cure, ZR-Cem™ will reach a gel phase in 1-1:30 minutes. In either case, during the gel phase ZR-Cem™ is easily peeled away from the margin ensuring complete removal of excess cement. This avoids the need for a bur to remove excess cement, which may traumatize surrounding gingiva and damage the new restoration.
ZR-Cem™ has several other features that make it a unique SARC. First, the adhesive monomer 10-MDP is included to facilitate a strong bond to all crown and bridge materials, especially zirconia. It also features a novel catalyzing system that is benzoyl peroxide and amine-free, which helps ensure excellent color stability and eliminates the need for refrigerated storage.
ZR-Cem™ is supplied in 8 gram dual-barrel automix syringes and is available in translucent, A2, and White shades.
Clinical Case
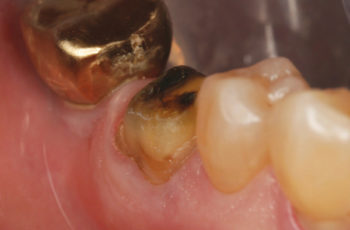
Fig 2. Final preparation of tooth No. 30 after removal of older porcelain fused to metal crown.
Approximately three weeks after removing an existing porcelain fused to metal restoration on tooth No. 30, the patient returned for final delivery of a monolithic zirconia crown (Fig. 2). The provisional and any excess cement were removed and the new crown was tried in to adjust interproximal contacts, occlusion, and esthetics.
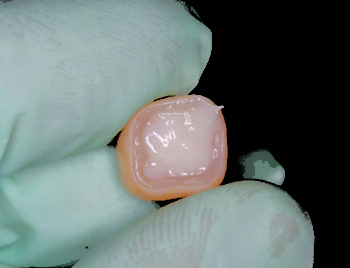 Fig 3. After bleeding the ZR-Cem™ twice (without the mix tip, and through the mix tip), crown No. 30 was filled with the cement. |
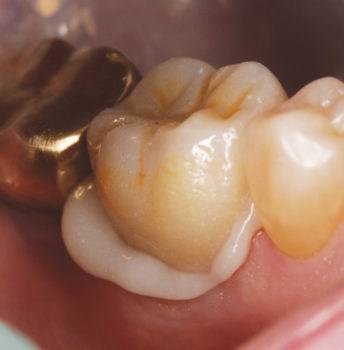 Fig 4. Zirconia crown No. 30 is seated on the clean and slightly moist preparation, excess cement is expressed. Note: no additional bonding steps of the tooth or pretreatment of the restoration are required prior to using ZR-Cem™. |
|---|
After sandblasting the intaglio of the restoration, the ZR-Cem™ translucent shade cement was prepared for use by bleeding the dual-barrel automix syringe prior to attaching a mix tip, to ensure both base and catalyst were expressing evenly. Then, the mix tip was installed and a small amount of material was dispensed onto a mixing pad to again ensure adequate mix of the cement components. Without delaying, ZR-Cem™ was dispensed into the crown directly from the mixing tip, followed by immediately seating it onto the clean and slightly moist preparation (Fig. 3 & 4).
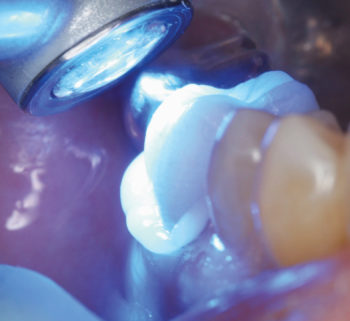
Fig 5. Tack-curing of the ZR-Cem™ was accomplished by three seconds of light curing to both the buccal and lingual surfaces.
The buccal and lingual aspects of the restoration were tack-cured for 3 seconds each using a Smartlight® Focus® Pen-Style LED Curing Light (Dentsply Sirona), initialing a gel phase (Fig. 5).
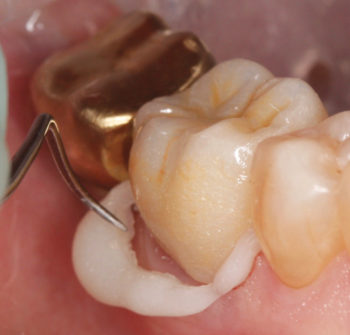
Fig 6. After tack-curing, ZR-Cem™ in the gel phase peels away easily from the margins of the
restorations, helping to ensure no excess cement is left behind.
The cement was gently removed using an explorer; great care was taken to avoid causing gingival bleeding (Fig. 6). Interproximal excess was removed by stabilizing the restoration and flossing the areas; horizontally removing the floss after each area was verified.
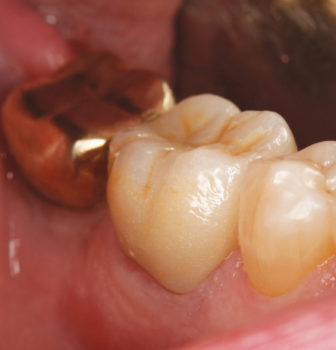
Fig 7. The final restoration on tooth No. 30 immediately after definitive cementation with ZR-Cem™ Self-Adhesive Universal Resin Cement.
After successful removal of excess cement, the restoration was stabilized by having the patient bite on a cotton roll until final set of the cement occurred (four minutes from the start of mixing). At this point, final verification of interproximal contacts, occlusion, and esthetics was completed and the patient was released (Fig. 7).

Jason H. Goodchild, DMD is the Vice President of clinical affairs, Premier Dental Products Company, Plymouth Meeting, Pennsylvania; an associate clinical professor, Department of Oral and Maxillofacial Surgery, Creighton University School of Dentistry, Omaha, Nebraska; an adjunct assistant professor, Department of Diagnostic Sciences, Rutgers School of Dental Medicine, Newark, New Jersey; and in private practice in Havertown, Pennsylvania. He can be reached at: JGoodchild@PremierDentalCo.com.
Published in TIPS – March/April, 2020. Submitted by Premier.
Category: Merchandise
Back to Articles