Severe Bone Loss Around Teeth #24 and 25 with Class 3 Mobility and Secondary Occlusal Traumatism
The major drawback to BIS-GMA provisional has been insufficient strength and durability for when a patient will not be able to afford a permanent crown for several years, or for longer term interdisciplinary cases requiring periodontal or implant procedures. The latter situation is exemplified by the following case in which the use of LuxaCrown (DMG) made it possible to create a long-term restoration that would easily last until an implant procedure was possible.
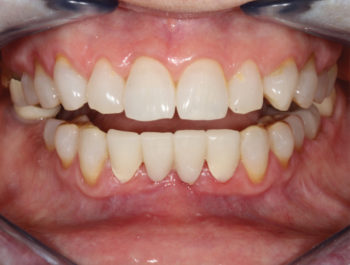
A healthy 65-year-old woman was finding it increasingly difficult to bite on her front teeth. Her full exam revealed severe bone loss around teeth #24 and #25 with class 3 mobility and secondary occlusal traumatism (Fig. 1A). The prognosis did not allow the teeth to be saved, so atraumatic removal was recommended. Treatment planning with a CBCT showed a damaged buccal plate (class 3 defect) that would compromise immediate implant placement indicating that 2 stage grafting/implant surgery was needed. The patient wanted a stable fixed transition solution while healing from her procedure. In addition, an ovate pontic design would preserve the gingival architecture by providing a “scaffold’ to prevent collapse and flattening of the papillae.
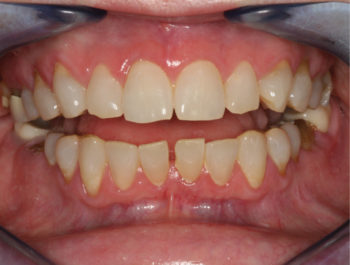 1A – Spacing between lower incisors contributing to difficulty eating and chewing. |
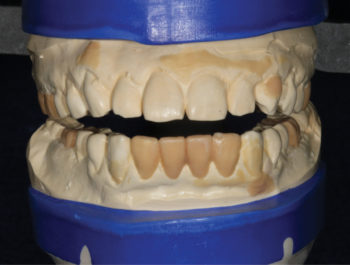 1B – Blueprinting a final outcome to establish functional esthetic parameters. |
|---|
Prosthetically driven care requires blueprinting a final outcome to establish functional esthetic parameters that fulfills patient desires. A well designed and sculpted putty matrix was provided by the laboratory to transfer the details to the mouth (Fig. 1B). On the day of surgery, the patient was pre-medicated with a sedative dose of Xanax. Eight vials of blood were drawn to create a mix of PRGF and 50/50 mix of cortical/decortical bone for optimal bone enhancement. After anesthetic infiltration, teeth #23 and #26 were prepared to allow for a fixed transitional bridge. The central incisors were atraumatically luxated to spare any remaining bone, and the sockets were carefully debrided and irrigated with sterile saline. LuxaCrown was injected into the putty matrix and intraorally around the gingival tissues to create precision margins and ovate pontics (Fig. 1C). The prosthesis was shaped with discs and composite finishing burs. It was readily apparent that the firmness of the material reflected its higher density. Occlusion was refined in centric and eccentric positions. Final polish was done with 3 grits of discs and aluminum oxide paste (Fig. 1D) and the bridge was placed in Peridex.
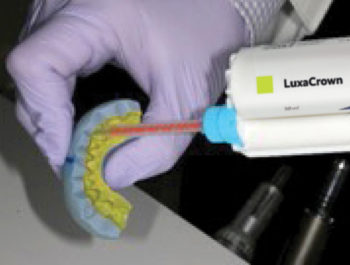 1C – Luxacrown injected into putty matrix and around gingiva to create precise margins and ovate pontics. |
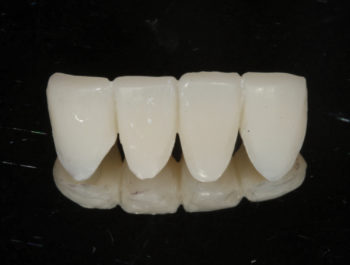 1D – Final polish done with 3 grits of discs and aluminum oxide paste. |
|---|
Following stimulation of the socket bone, the intraosseous bone graft was placed and packed into the extraction sites. Figure eight suturing with self-resorbing 4-0 Polyglycolic Acid (PGA) was performed to hold the tissues and graft material stably for 60-90 days. The provisional was cemented carefully after coating the preparation with a disinfectant and desensitizer, followed by a reversible cement (Fig. 1E). Flossing was discouraged around the pontic sites to avoid disrupting the healing response.
The patient was ecstatic about the rejuvenated esthetic and functional improvement of her lower teeth. The stability and firmness gave her and her dental team the peace of mind that new prosthesis would be durable during the tissue healing process and future implant care. Biologically, the high polish and precise adaptation around the tissues enabled the papillae to remain intact at the 45-day post-o perative mark (Fig. 1F). Such an outcome was not possible with standard BIS-GMA materials.
 1E – Provisional cemented after coating preparation with disinfectant and desensitizer. |
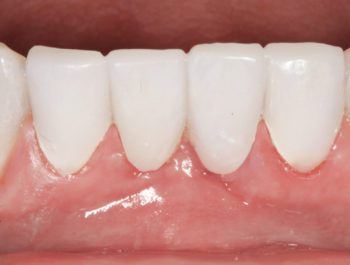 1F – 45-day high post-operative image shows high polish and precise adaptation around tissues. |
|---|
Written by Dr. Hugh Flax, DDS, AACD, MICOI, DABAD
Permission to publish provided by DMG America.
Published in Catalyst – Spring/Summer 2020.
Category: Merchandise
Back to Articles